#40 - The $1.8 Billion Toddler
Devoted's big raise, NY might challenge CVS-Aetna, and more from this week in healthcare
Things That Happened

Devoted Wealth. Todd and Ed Park, DJ Patil, Bob Kocher, and the rest of the team at Devoted Health are such a dream to investors that they announced this week they’ve raised a $300m series B and started enrollment on their first Medicare Advantage plan. And CNBC reported they’re doing so at a $1.8 billion valuation. They’re a unicorn while being just 19 months old, and before they’ve earned a dollar in revenue. This is either a once-in-a-generation company, or a sign of overly exuberant venture capital. Either way, it’ll be fun to watch what happens.
UHC PHR TBA. UnitedHealth Care is planning to launch a personal health record for its members. I’m convinced that most people will one day use a PHR to view their clinical records and log their health tracking data, but I’m not sure it makes sense for that PHR to be tied to a health plan. Health plans come and go as we move and change employers. This could be one reason Apple’s externality to the system is actually a benefit in the PHR game - a consumer’s relationship with his iPhone has nothing to do with his employer or location.
$931 million. That’s how much a group of compounding pharmacies and their telehealth conspirators tried to bilk out of insurance companies. They have been indicted. Even when it comes to fraud the numbers always seem to be bigger in healthcare.
HackCare.gov CMS reported this Friday evening that they’ve detected “suspicious activity” on the agent & broker portal of healthcare.gov. 75,000 individuals’ files were improperly accessed.
PhRMA makes a reasonable point. In anticipation of regulations requiring drug advertisements to include the list price of the drug, PhRMA has announced their plan to voluntarily feature list prices for drugs on a website. It would also include what a patient is likely to have to pay for the drug. Their point: the list price is meaningless as nobody actually pays it. They’re not wrong.
The Empire State Strikes Back. The New York State Department of Financial Services is signaling they might block the merger of CVS and Aetna’s New York businesses because the DOJ didn’t do enough to protect consumers when approving the deal.
Things Worth Understanding
My first job in healthcare was working as an analyst at a strange little startup. Our goal was, for those elective procedures with the right economics, to help providers better manage their capacity through offering discounted pricing at times of the day and week that were usually much slower. This would create a two-sided marketplace where patients could find discounted prices for elective procedures, and where providers could gain more business simply by changing pricing and hours.
This was right when the notion of the lean startup was taking hold. While our office was in a sleepy commercial park off a busy highway in Northern New Jersey, we decided to act like one of those fast-moving Bay Area startups.
We built a consumer-facing website where customers could see a list of providers and their pricing ranges, and request appointments. We’d be notified once a customer placed a request, and then we’d pick up the phone and get in touch with the provider to book an appointment at the requested price.
While the company floundered fairly quickly for a variety of reasons, my time there gave me a chance to become intimately acquainted with the relationship of technology to innovation. More specifically, I learned not to confuse business model innovation with technological innovation.
I watched as, in relatively short order, we were able to launch our service without building more than a basic website. We were able to deliver on our two-sided value proposition, filling exam rooms and getting patients cheaper care, without building a complex system or hiring an army of software engineers. Our value was delivered without inventing anything other than a new process for connecting patients and providers.
The problem, as I’m sure you see it without me spelling it out, was that our manual, phone-based process wasn’t going to scale. There’s no way the small matchmaking fee we took for booking an appointment would cover the labor cost of doing the work to set it up. There wasn’t enough meat on the transaction for us to take a big enough bite while leaving enough to keep the other parties coming to the table. That’s where the tech comes in.
Technology enhances processes. It can take processes we’re already doing, automate them to reduce or remove human labor, and make things generally faster and more efficient. It can transform variable cost into fixed cost, enabling business models that were previously economically inviable. Once we’d built a system that could automatically match patient demand to provider capacity, our business would be able to scale as quickly as we could feed it customers and suppliers.
This may seem patently obvious, but it’s important to remind ourselves that in a world that prizes tech above all else, you have to first create the model, then apply tech to automate your way to it being viable. You can’t simply throw technology at utterly broken systems and hope everything starts to work as it should.
This is especially important in healthcare because the system is especially broken. Electronic Health Records haven’t done anything to make physicians’ lives easier because all they do is reinforce a system that wasn’t working well in the first place. Conversely, you can look at solutions like Sherpaa, which uses technology to enable a 100% virtual and asynchronous relationship with your primary care doctor, but hasn’t taken off because it exists outside of our existing payer-provider ecosystem.
Introducing technology into a broken system will only perpetuate and magnify systemic failures. You have to fix the system first, then introduce technology to make it sing.
Things To Read
Does the CVS-Aetna merger really deserve all this scrutiny? Not really, if you’re okay with all the other large corporations that have already vertically integrated. Josh Barro examines vertical mergers in healthcare, noting that they can even sometimes end up benefitting the consumer.
At a basic level the explanation of how these mergers actually help patients is similar to that of an Accountable Care Organization: by combining payer with provider, the payer gains more control and greater incentive to optimize service utilization and the cost of delivering care. I’d be more interested in seeing this responsibility growth occur in terms of time - how would a payer’s incentives change if policyholders were on 5 year contracts instead of 1 year contracts?
“61% of digital health companies that start B2C end up pivoting to B2B and selling to insurance companies, employers, hospitals, or other healthcare providers.” Paul Yock explains how mainstream tech’s standard-operating-procedure of iterative product development and a healthy consumer obsession can actually serve as a hindrance in the world of healthcare. The difficulties flow from the fact that in healthcare the standard functions of a consumer - selecting a product, using a product, and paying for a product - are actually completed by three different parties: providers, patients, and payers.
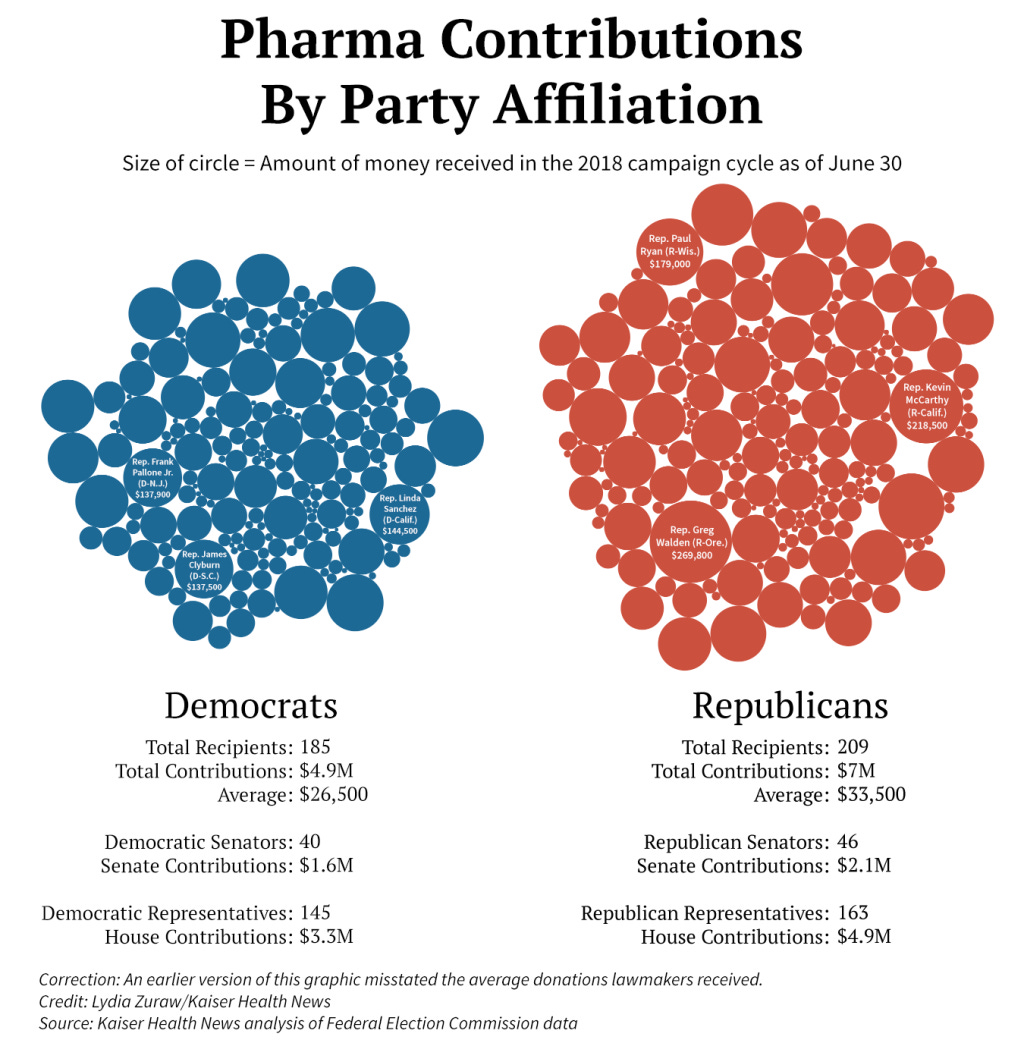
How much money does pharma send to Washington DC? Sydney Lupkin and Emmarie Huetteman explore pharmaceutical companies’ campaign contributions, PAC donations, patient advocacy, and lobbying spends in this piece in Kaiser Health News. KHN also has this handy database where you can easily see how much money your Congressman or Senator took from pharma companies, if you’re interested in that sort of thing.
“What is the difference between 300 apps on the app store versus a digital therapeutic?” That’s Pear Therapeutics CEO Corey McCann asking what I’m sure he hopes will one day be a rhetorical question. Digital therapeutics companies are creating software tools designed, and FDA approved, to treat specific behavioral and mental health conditions. But they must regularly sell themselves as something beyond the slew of wellness apps that fill the app store. A helpful mental model suggested by McCann: digital therapeutics are to wellness apps what pharmaceutical drugs are to dietary supplements. Read more from Jonah Comstock’s coverage of the Digital Health Innovation Summit.
“researchers report that by testing the 1.28 million samples contained in a consumer gene database, they could match 60 percent of the DNA of the 140 million Americans of European descent to a third cousin or closer relative.” Technology is enabling researchers - and others - to glean deeper information than previously possible from genetic databases. Read Paul Raeburn’s piece in Scientific American for more on how you can be found in a genetic database even if you’ve never volunteered your DNA.
The rumors are true: Medicare actually is more efficiently administered than private plans. But if Medicare For All were to come to fruition, policyholders might find the services they receive lacking compared with private insurance plans. Austin Frakt unpacks Medicare’s economics for the NY Times.
Thanks for reading The Healthcare Handout, a weekly update on tech and business in healthcare from Isaac Krasny. Criticize, praise, hire, or otherwise get in touch with Isaac via isaac@healthcarehandout.com, or on twitter @isaackrasny
And remember, this machine runs on sharing. If you found this newsletter informative or thought-provoking, give it a boost by sharing with a friend or colleague. Or share a testimonial.


